HIV
The Connection Between HIV and Osteoporosis
HIV is a crippling disease that slowly but surely tries to break down your body’s defenses. The virus compromises your immune system and your ability to fight off infections, leaving you vulnerable to the diseases of the world. One such condition includes osteoporosis.
Osteoporosis is a condition that affects both men and women over the age of 50. More than 4 percent of men and 16 percent of women over the age of 50 live with this disease in their femur neck or lumbar spine. To make matter worse, those with HIV are more likely to develop osteoporosis and scientist are unsure why.
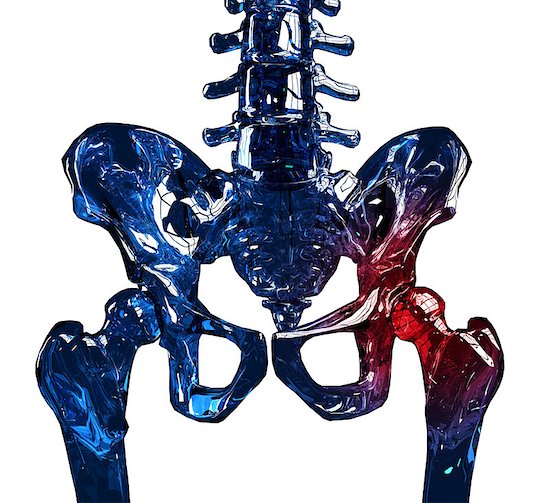
How Osteoporosis Affects the Body
The bones are the structure and frame of our body, allowing us the ability to move. Strong and healthy bones are needed to keep the body upright, moving, and working properly. When osteoporosis strikes, the bones in our body begin to hollow out. This loss of bone density and mass causes bones to become weaker, leaving them susceptible to breakage.
Severe cases are known cause damage when a person sneezes or receives a minor bump. The longer a person has osteoporosis, the more likely they are to experience hip fractures, a collapsed vertebra, severe back pain, a loss of height, and spinal deformities.
How Are the Two Diseases Connected?
Over 54 million Americans live osteoporosis, while 1.2 million have HIV. Many studies show that the two disease are somehow connected. The loss of bone density occurs faster in those with HIV. What scientists don’t know is the exact cause. However, that hasn’t stopped them from trying to figure out why patients with HIV develop osteoporosis. The most common theories are the following:
- HIV medications.
- Long-term use of other medications like blood thinners, an antiseizure medicine, and corticosteroids.
- Old age.
- HIV infection.
What Symptoms Should You Look For?
Unfortunately, it can be hard to determine if you have osteoporosis unless you have broken a bone. This symptom the first sign of the disease. The U.S. Department of Health and Human Services (HHS) recommends bone density test for women over the age of 65, as they are the most at risk for the disease.
If you are HIV positive and over the age of 50, you should get tested as well. It’s important to look out for strain in your bones and joints, as well of any abnormal pain in those areas caused by a sudden bump or fall.
Preventing Osteoporosis
If you are HIV positive but do not have osteoporosis, there are measures that you can take to prevent the disease. A healthy diet will replenish the nutrients you need to maintain healthy bones. Be sure to eat plenty of foods with calcium and vitamin D. A healthy lifestyle will also slow the rate of bone loss. Exercise often and cut out bad habits like smoking and drinking alcohol. The most important thing that you can do is see your doctor or HIV specialist. An expert can guide you and the risk and steps to dealing with HIV and disease like osteoporosis.
The Sneaky Nature of the HIV Virus
There is no doubt that HIV is a deadly virus. Since it was discovered, this pandemic has infected 78 million people and 35 million have died due to an AIDS-related illness. The worst part is that scientists have yet to find an absolute cure to the disease. Why is it that the HIV virus is so hard to eradicate? What is it about the disease that makes treatment difficult?
Many experts note the infection’s ability to hide within the body. HIV is notorious for eluding even the most powerful combinations of medicine. The sneaky nature of the disease allows it to wait until the right moment, when the body’s defenses are down, to attack the immune system. Even today, scientists are still trying to figure out and understand exactly how the virus works in order to combat its effects on the body.
How the HIV Virus Moves Within the Body
Once the body is infected with HIV, the virus begins to attack the immune system. It’s number one target are the CD4 cells in the body. These cells help the immune system fight off infection and diseases. Little by little, HIV lowers the CD4 count until the body can no longer protect itself.
The best defense against HIV is antiretroviral therapy (ART). This is a combination of several medications that work together to suppress HIV levels in the body. In order for this treatment to work, it has to be taken daily. When taken properly, the treatment has proven effective in reducing traces of the virus to nearly undetectable levels and preventing the progression of the disease to aids.
What Studies Have Found
ART is no cure. Traces of the virus remain within the body despite the use of these strong medications. The virus likes to hide in immune cells when at low levels. By remaining dormant in these “Sanctuary Sites,” it can wait in places unreachable by drugs. Once it has found the right moment, it will quickly reproduce when an HIV positive individual stops taking ART therapy.
In a recent joint study by the Monash Biomedicine Discovery Institute and the Systems Immunity Research Institute at Cardiff University, the two institutions discovered that mutations within HIV help it appear dormant and virtually undetectable by the immune system. These mutations change the way that key immune molecules called Major Histocompatibility Complex (MHC), display the virus.
“This work uncovers a novel mechanism for HIV immune escape, which will be important to incorporate into future vaccine development and may have broader implications for immune recognition of MHC molecules,” he said.
What You Can Do
While scientists work hard to find a way to detect and eradicate the HIV virus completely, you have to do your part to curb the spread of the virus. Protect by getting tested. Knowing is an important step. If you are HIV-negative, protect yourself by practicing safe sex and taking pre-exposure prophylaxis (PrEP). For those infected by the disease, remember to take ART daily to prevent the virus from progressing.
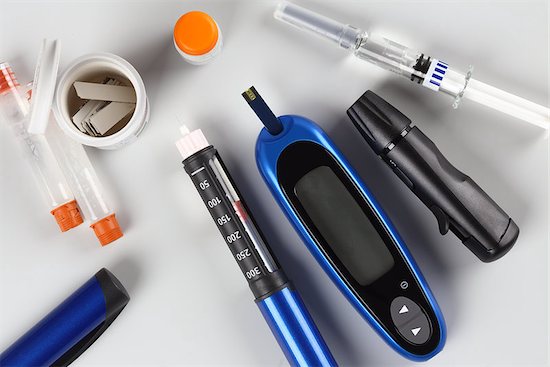
Diabetes Risk: HIV Patients Have a Higher Risk
Patients with HIV are always at risk. They are left vulnerable to infections and other comorbidities due to the virus attacking their immune system. Scientists were startled when they made the revelation that HIV patients had a 4 percent higher risk of developing diabetes. This discovery was made in a recent study published in the BMJ Open Diabetes Research & Care online journal.
Despite Low Obesity Rates, Diabetes Risk Persist
Obesity is a key indicator of diabetes. However, many patients with HIV do not have obesity, a fact leaving scientist confused. To find out just how prevalent diabetes is among the HIV population, researchers launched a probe into two sets of data from 2009-2010.
They analyzed a survey of 8,610 HIV-positive individuals in the Medical Monitoring Project (MMP) and another survey of 5,064 people without the disease who participated in the annual National Health and Nutrition Examination Survey (NHANES). Comparing these two sets of data would give them insights into the diabetes risk of those with and without HIV.
Here is the breakdown of what the researchers found:
- One in 10 HIV patients had diabetes.
- 4% of those with diabetes had type 1.
- Over of those with diabetes had type 2.
- 44% of HIV patients had and unspecified strain.
- Over 8% of the general population had diabetes.
- The occurrence of diabetes was 3.8% higher in HIV patients.
This study was able to show that HIV patients are at risk. However, since the research was purely observational, scientists were not able to make a definitive conclusion as to why. They know that obesity is still a risk factor, but due to its high absence in individuals with HIV, they have to think differently.
The researchers had this to say: “Additional research would help to determine whether [diabetes] screening guidelines should be modified to include HIV infection as a risk factor for [the condition], and to identify optimal management strategies in this population.”

Inspirational HIV Quotes That Promote Positivity
For this post, we’ve decided to do something a little different and share our favorite inspirational HIV quotes. Living with HIV is a day-by-day challenge. Because of this, a positive mindset is important. High anxiety and depression have a strong effect on HIV patients. More so than a regular patient.
People with HIV want to be treated with kindness and respect. Just like everyone else. Telling them as much can go a long way. So, with that in mind, here are just a few of some of the most inspirational HIV quotes.
Inspirational HIV Quotes
- “Being seen does have value. I have the support of my boyfriend, my great friends, and my loving parents. Many do not and this is, in part, for them.” – Olympian Ji Wallace on having HIV.
- “We need to band together as a unit every day, especially to conquer the strength of the AIDS virus.” – Actor Dustin Hoffman, on combatting the spread of HIV/AIDS.
- “HIV does not make people dangerous to know, so you can shake their hands and give them a hug: Heaven knows they need it.” – Princess Diana, on getting rid of the HIV stigma.
- “Sick people, particularly those with serious conditions, greatly prefer the company of their friends and family to residence in a hospital or nursing home.” – Author and activist David Mixner, on the importance of a strong support system for sick people.
- “Three decades into this crisis, let us set our sights on achieving the “three zeros.” Zero new HIV infections, zero discrimination, and zero AIDS-related deaths.” – Ban Ki-Moon, secretary-general of the UN, calling for the cure of HIV and AIDS.
- “We live in a completely interdependent world, which simply means we cannot escape each other. How we respond to AIDS depends, in part, on whether we understand this interdependence. It is not someone else’s problem. This is everybody’s problem.” – Bill Clinton, discussing a united front in solving the AIDS crisis.
Some of the most iconic figures of the past century have shared inspirational words about HIV. Whether the person is royalty, a writer, or even a Hollywood star, they all share the same eagerness when it comes to fighting HIV. They believe that positivity, as well as working together, will help find a cure to end the virus once and for all.

Improving Linkage to Care is the Next Goal for HIV Treatment
Linkage to Care (LTC) is the three-month period of time between diagnosis and medical treatment for HIV. Groundwork is laid for future treatment during this time. Newly-diagnosed patients need to understand the ins and outs of their diagnosis. It’s a crucial part in such a transitional time in their lives.
Studies have shown a wide range of information regarding how many HIV patients are getting LTC. The number is often between 59% and 80%. Many consider this to be too low a number either way. This has prompted more developed nations to set their Linkage to Care rate to 90% by 2020.
The World Health Organization (WHO) stresses the importance of providing a service built around the health needs of those living with HIV. A diagnosis of this magnitude can make a patient feel vulnerable. Consequently, WHO believes treating them with dignity goes a long way.
WHO recently gave a list of suggestions that studies suggest would help improve LTC. Here is what they find to be most helpful.
Steps to Help Increase Linkage to Care
- Streamlined interventions to reduce the time between diagnosis and engagement in care. This includes enhanced linkage with case management and support for HIV disclosure.
- Carrying out routine viral load testing 6 months and 12 months after Antiretroviral Therapy (ART). If the patient is stable on ART, then every 12 months would be all that’s necessary.
- Improving the data used to identify the linkage’s quality.
- Less frequent clinic visits for those stable on ART. As a result of ART working for them, every 3-6 months would be sufficient.
- Programs that provide community support boosts retention in care. Methods suggested for them to use include: interventions, peer counselors, and mobile communication.
When Linkage to Care is initiated early for HIV patients, better medical treatment is possible. Increasing the amount of people who receive earlier treatment is a great first step in managing the disease.