Posts tagged Antiretroviral drugs
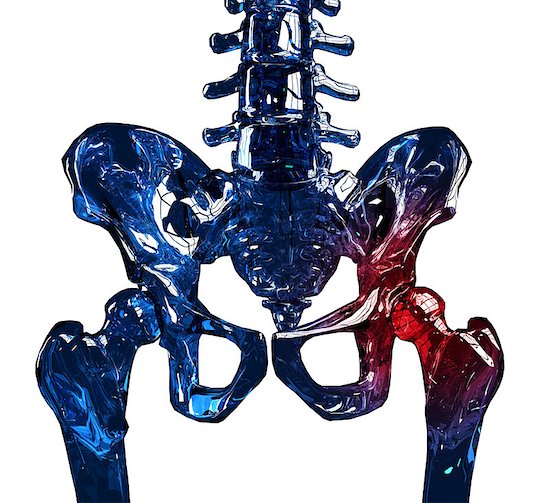
The Connection Between HIV and Osteoporosis
HIV is a crippling disease that slowly but surely tries to break down your body’s defenses. The virus compromises your immune system and your ability to fight off infections, leaving you vulnerable to the diseases of the world. One such condition includes osteoporosis.
Osteoporosis is a condition that affects both men and women over the age of 50. More than 4 percent of men and 16 percent of women over the age of 50 live with this disease in their femur neck or lumbar spine. To make matter worse, those with HIV are more likely to develop osteoporosis and scientist are unsure why.
How Osteoporosis Affects the Body
The bones are the structure and frame of our body, allowing us the ability to move. Strong and healthy bones are needed to keep the body upright, moving, and working properly. When osteoporosis strikes, the bones in our body begin to hollow out. This loss of bone density and mass causes bones to become weaker, leaving them susceptible to breakage.
Severe cases are known cause damage when a person sneezes or receives a minor bump. The longer a person has osteoporosis, the more likely they are to experience hip fractures, a collapsed vertebra, severe back pain, a loss of height, and spinal deformities.
How Are the Two Diseases Connected?
Over 54 million Americans live osteoporosis, while 1.2 million have HIV. Many studies show that the two disease are somehow connected. The loss of bone density occurs faster in those with HIV. What scientists don’t know is the exact cause. However, that hasn’t stopped them from trying to figure out why patients with HIV develop osteoporosis. The most common theories are the following:
- HIV medications.
- Long-term use of other medications like blood thinners, an antiseizure medicine, and corticosteroids.
- Old age.
- HIV infection.
What Symptoms Should You Look For?
Unfortunately, it can be hard to determine if you have osteoporosis unless you have broken a bone. This symptom the first sign of the disease. The U.S. Department of Health and Human Services (HHS) recommends bone density test for women over the age of 65, as they are the most at risk for the disease.
If you are HIV positive and over the age of 50, you should get tested as well. It’s important to look out for strain in your bones and joints, as well of any abnormal pain in those areas caused by a sudden bump or fall.
Preventing Osteoporosis
If you are HIV positive but do not have osteoporosis, there are measures that you can take to prevent the disease. A healthy diet will replenish the nutrients you need to maintain healthy bones. Be sure to eat plenty of foods with calcium and vitamin D. A healthy lifestyle will also slow the rate of bone loss. Exercise often and cut out bad habits like smoking and drinking alcohol. The most important thing that you can do is see your doctor or HIV specialist. An expert can guide you and the risk and steps to dealing with HIV and disease like osteoporosis.

The Progression of HIV: How the Infection Takes Over Your Body
It’s important to know every aspect of HIV, in particular for those infected with the virus. HIV is a volatile disease and an epidemic that has claimed the lives of over 35 million people. Understanding how the disease works can help patients make better decisions when it concerns their health. That’s why it’s imperative that patients are informed because over time and without proper treatment, HIV develops into something much worse. Find out everything you need to know about the progression of HIV and how you can protect yourself.
Laying Out the Progression of HIV
HIV progresses in three stages. As the disease moves from one stage to the next, it becomes worse over time. Eventually, the disease completely eradicates the immune system, leaving the body vulnerable to other diseases and infections. Let’s walk through the different stages of the virus and what it means for HIV-positive individuals.
Stage 1: Acute HIV Infection
The progression of HIV starts soon after infection. The first stage of the virus is known as acute HIV infection. During this stage, symptoms aren’t noticeably apparent, and for the first 2 to 4 weeks, people may be unaware that they have contracted the disease. There is a chance that HIV-positive individuals experience flu-like symptoms. These symptoms are a telling sign for anyone who has recently participated in risky sexual activity or drug use. It usually means that they have contracted the virus and it has start to multiply, causing it to spread within the body and destroy the immune system.
Stage 2: Clinical Latency
As defined by the CDC, Clinical Latency is the second stage of the virus. It is also known as asymptomatic or chronic HIV infection. While still active within the body, the HIV virus reproduces at low levels. Most people still do not show any symptoms of the disease by this point. However, it is important to note that one can still spread the infection to others. This stage is also a crucial period as the disease can evolve and become AIDS without proper treatment.
Stage 3: AIDS
AIDS is the final stage of HIV. This is when the number of CD4 cells in the body, which aid the immune system, are at their lowest. AIDS grants other infections and diseases the opportunity to damage the body severely. Your symptoms often depend on the type of illness or opportunistic infection you contract. This stage can occur when one has not properly taken medication during the first or second stage of the virus. Patients with AIDS who continue to ignore treatments usually live for three years.
Slowing Down the HIV Infection
While there is no cure for HIV, scientists are working diligently every day to find one. Their research has led to advancements in HIV medications. By taking this treatment, patients can slow the progress of the disease. Some have even found success in keeping it at stage 2 for many years, preventing the transition to AIDS. For this treatment to be effective, patients must take the antiretroviral medications every day. If you are worried or concerned that you may have contracted HIV, contact an HIV specialist today and get tested as soon as possible.

Hypertension an Increasing Problem for Africans Living With HIV
HIV is a worldwide epidemic. From country to country, the virus has a significant impact. This makes it harder to provide the resources to fight against the virus. In sub-Saharan Africa, there were 24.7 million people living with HIV in 2013. Even worse, the number of new HIV infections are up to 1.5 million. Only 39% of adults receive antiretroviral treatment.
At-Risk Individuals
There are several key groups affected by HIV within this region of the world. Unfortunately, research has shown that many of the countries in Africa, mainly Southern Africa, are the worst affected by the disease. The government continues to encourage and offer more testing for the population but many individuals are unaware of their status, leaving the country at continued risk.
The groups who are the most at risk included young women, children, sex workers, men who have sex with men, and drug users. There are several factors putting these groups in danger. Condom distribution varies from country to country. It is also not uncommon to find younger women in relationships with older men. More than 4 in 10 new infections are young women around the 15-24, who are participating in unsafe sexual behavior.
Hypertension and Living With HIV
A new problem has risen in the region of sub-Saharan Africa. Scientists are discovering a high prevalence of hypertension among rural Africans. New research reveals that about 12 percent of people living with HIV in Tanzania have hypertension when they are diagnosed. Furthermore, an additional 10 percent of the population will develop Hypertension during the first months of antiretroviral therapy.
Tanzania has approximately 1.4 million people living with the virus. However, the country has done well to curb the spread of disease. New infection dropped by more than 20% between the years of 2010 and 2015. This is due in part to the increase of antiretroviral drugs in the area.
The researchers note that the development of hypertension in these patients is likely in relations to normal cardiological risk factors like age, body mass index, and renal function. The effect that antiretroviral drugs have on the body may play a role, though.
How Scientists Plan to Address the Issue
The prevalence of HIV and hypertension is 1.5 times higher than both Europe and the United States. This is trouble for a region that is already dealing with this epidemic. Dr. Emilio Letang, Swiss TPH and Barcelona Institute for Global Health (ISGlobal) has a few suggestions to combat the combination of both conditions.
“We have seen that such routine screening is a feasible and effective strategy to diagnose hypertension within an HIV programme. Moving forward, however, we need to make sure that leveraging such synergies does not compromise the efficiency of existing HIV programmes,” says Dr. Emilio.
Prof. Dr. Christoph Hatz, Chief Medical Officer at Swiss TPH continues by stating that “In many countries across sub-Saharan Africa, there is still a lack of access to drugs against major non-communicable diseases. In order for such integrated care programmes to work successfully, ensuring better availability and affordability of drugs as well as implementing comprehensive preventive and curative measures will be key.”

Computer Analyzes Adverse HIV Drug Effects
Drugs are often a double-edged sword. While their purpose is to cure or alleviate symptoms caused, many of them come with complications. This is often the case with drugs for severe conditions such as HIV drugs.
Furthermore, HIV is one of the most troublesome diseases in the world. Medications help fight off the virus but they can also have adverse effects on the body. One of the most common drugs for HIV is abacavir. The side effects of this drug are rare but a certain portion (5 to 8 percent) of patients do experience an intense allergic reaction to it.
Abacavir is known to cause hypersensitivity syndrome. This is a life threating reaction which can cause fever, rash, nausea, vomiting, diarrhea, and abdominal pain. If patients have a particular human leukocyte antigen (HLA), these symptoms usually appear within the first two to six weeks of taking the HIV drug.
The HLA protein is a substance that induces an immune response. These proteins are located on the surface of a cell and often communicate with T-cells. If an entity other than a co-binding peptide binds to an HLA protein and changes it, the protein will deem it foreign. This signals the T-cells, and cause an immune response. Often, the abacavir drug appears as an unknown entity when it tries to bind to the cells.
Researchers Take a Closer Look at HIV Drug
A test was performed at North Carolina State University. Researchers used a computer model to get a closer look at the abacavir drug reaction on a molecular level. They wanted to see the drug’s interaction with the HLA proteins.
“There are 15,000 variants of HLA, and everyone carries some of these variants,” says Denis Fourches, assistant professor of chemistry at NC State. “HLA-B*57:01 is one of the first variants studied in the context of a drug-induced immune reaction. We know that it binds with abacavir, but little was understood about exactly what was happening structurally at the molecular level, especially in terms of the relationship with the co-binding peptide. This is a very complex system.”
The computer was able to create 3D models of the HLA protein, abacavir, and the co-binding peptides. Researchers simulated the docking process with and without co-binding peptides. They also ran simulations of the process with 13 other HIV drugs that have similar effects.
“The models allowed us to identify key atomic interactions that cause abacavir and other drugs to bind to the HLA variant protein and ultimately trigger the immune response,” Fourches says. “When you can forecast and understand the elements of the drug that enable the binding to occur, you may be able to create new active compounds that do not have that problem.”
The research team at NC state hopes that his in-depth look at binding process will provide them a better understanding of how the immune system reacts to drugs. With this knowledge, they can predict the side effects of medications. In the future, they can also build better drugs. Hopefully, they will avoid life-threatening situations.

Better HIV Treatment Leads to Riskier Behavior in Gay Men
The advancements in HIV treatment have made it easier to stall the progression of the virus. However, a new study suggests that the news of these treatments is having an unintended consequence. More gay men are engaging in risky behavior because they believe that antiretroviral medicines will keep them safe. However, the continuation this kind of behavior only increases their risk despite taking proper prevention methods.
The Risk to Gay Men
Gay Men are already more likely to contract HIV than others. In 2015, gay and bisexual men accounted for 67 percent of all new diagnoses. Anal sex is the highest risk factor for HIV transmission. Receptive anal sex puts more men at risk than insertive anal sex. This is because of the rectums thin lining, which allows HIV to enter the body more easily. The transmission of HIV can happen from semen or pre-seminal fluid.
The Danger of Relying Solely on Medicinal HIV Treatment
Study leader Seth Kalichman of the University of Connecticut and his team analyzed a survey spanning 19 years. Participants at a gay pride event noted their sexual habits. Here is what they found:
- An increase in condomless sex among men.
- A rise in the number of sexual partners that men engaged with.
- Condomless receptive anal sex has doubled in HIV-negative men.
- Condomless insertive anal sex has tripled in HIV-negative men.
We are seeing a considerable increase in unsafe sex because gay men perceive antiretroviral drugs to be enough. However, after looking at the survey data, they found there wasn’t much of a reduction of new HIV infections in major cities. In fact, certain countries with HIV testing programs and antiretroviral drugs have seen infection grow among gay men. The risk remains when unsafe behavior increases.
Kalichman concludes that “The current study adds to the mounting evidence that substantial changes have occurred in community-held beliefs that condomless anal sex is safer in the era of HIV treatment as prevention.”