Posts tagged HIV cure

Assessing the Average Life Expectancy With HIV
Studies have shown how a patient’s life expectancy with HIV has gotten better over the past 20 years. A lot of progress has been made. Researchers have found breakthrough treatment methods. And treatment itself has gotten more readily available.
It’s now well known that HIV is no longer a death march. Patients are now able to live fuller lives compared to previous decades. But how much longer are they expected to live for? And what factors lead to such vast improvements? Let’s take a closer look at that right now.
Life Expectancy With HIV Over The Years
From 1996-97, the death rate for HIV-positive people was at 7%. For people diagnosed with HIV, their average life span was typically 10 years. For 20-year-olds with the virus, it was higher. On average, they lived until 39. These numbers are now significantly better.
By 2006, that number jumped to 24 years. More than double the average from a decade previous. And a 20-year-old with HIV lived until 56 on average. That number is now in the high 60s. That leaves a separation of about 13 years between an HIV-positive and HIV-negative 20-year-old.
That’s the smallest gap in life expectancy between the two parties to date. It goes to show how far we’ve come in two decades. But that there’s still work to be done.
How Life Expectancy Has Improved
Antiretroviral Therapy (ART) was not yet readily available in 1996. That’s changed over the past two decades. As a result of there being easier access ART, it revolutionized HIV treatment. By preventing the virus from reproducing, ART is able to lower the viral load in the bloodstream. When successful, the viral load is so low that the virus is undetectable. HIV is still there. And it can still be spread to someone else. But there aren’t any symptoms.
Treatment is more effective across the board. Over half of those eligible for treatment are now receiving it. Also, Linkage to Care numbers continues to increase. The necessary work is being done.
In addition to being more effective, HIV treatment is now simpler, too. Fewer pills are needed. And there’s no longer a complex schedule to follow. A lot of patients can now take one pill a day and be fine. They work for a longer period of time and have fewer side-effects. It’s less likely for a patient to have to switch medications periodically.

HIV DNA Successfully Removed from a Living Cell
HIV treatments have dramatically improved in recent years. Combinations of antiretroviral medications target the replicating of HIV within the body. When taken regularly, many HIV-positive individuals can lead relatively normal and healthy lives. As beneficial as these treatments are, researchers are still looking into finding an actual cure for the disease. One reason: if treatment happens to be interrupted, the virus quickly makes a comeback, and the infection can progress to AIDS. This is due to the latent HIV DNA within the cells.
Without the medications to suppress the virus, the infected cells are free to reproduce. Removing these viral pieces from the infected cells, and other areas where they lay dormant, is what would eradicate the infection.
HIV DNA: Gene Editing Takes the Next Step
In line with this objective, one recent study has successfully removed the HIV DNA from infected cells. The team had developed a sort of gene editor. The system works by targeting the infected cells and removing specific segments of HIV’s genetic material implanted by the virus.
When first tested, results were positive, and had little-to-no adverse effects. The most recent trial included targeting HIV material in organ tissue and blood cells. After just a couple of weeks, every type of tissue showed signs of the viral genetic material being removed. The broad spectrum of tissues gives hope that further developments will yield lasting and effective results, especially if gene editing is used in conjunction with current therapies.
Researchers are confident that if used alone, it has the potential to eliminate HIV from the body. Added benefits may come from using it along with antiretroviral therapies. Suppressing the virus’ ability to replicate, and removing its DNA from infected cells (even latent ones), will ensure a clean sweep. Seeing as the gene editing is also a very flexible technique, it is possible to tailor it to target mutated forms of the virus—an issue that continues to impede progress.
While the results from this study have years of trials and testing to go, it shows that medical objectives in regard to HIV and HIV DNA are feasible.
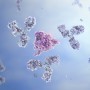
Using Antibodies in an Attempt to Find a Vaccine
The human immune system is a fascinating network capable of performing incredible feats. Even when HIV is involved, nearly one-third of individuals are capable of producing effective antibodies against the virus. Researchers have turned their attention to the antibodies produced during infection in order to facilitate the creation of an effective vaccine.
While some immune systems are adept at producing antibodies that act to neutralize a broad range of HIV strains, the process could, and often does, take up to a year before it is in full swing. Ideally, a vaccine should help a patient immediately combat the viral intrusion. This is one important goal for those developing vaccines. Efforts to speed up the process and make the antibodies available for everyone has prompted scientific study.
Certain effective antibodies were selected and closely examined. Of those, some had loop-like structures which, when they encountered the virus, were able to cling tightly and neutralize it. With the aid of computer modeling, modifications were made to the existing antibodies so as to maximize their efficiency. It is expected that such modifying will help increase the response time of the immune system, even if a person has never previously had contact with HIV.
Amino Acids Within Antibodies
Another aspect that was carefully reviewed was how the amino acids were sequenced in the antibodies that had proven most effective. Of the antibodies with a loop structure, certain ones had specific amino acid sequences that researchers tested and noted. A successful vaccine needs to provide adequate protection against more than just one or two strains of the tenacious virus. Those that were able to neutralize more strains were again plugged into the computer and modified. The re-engineering was to increase the capabilities of these powerhouse molecules.
Tests were also conducted to confirm that the alterations being made would, in fact, prove effective. The spectrum that the vaccine is designed to cover is wide, and when factoring in the potency of the design, researchers feel confident that if implemented, most people who are vaccinated would produce an effective response.
Promising Results in HIV Trials
The scientific community has relentlessly been in pursuit of an effective vaccine against HIV infection. With a competent vaccine in the arsenal, researchers could buy time to find a cure. Not only that, prevention is one way to curb its spread and help contain the disease. New information on the virus is discovered on a regular basis. Putting the facts together to formulate a line of defense has taken patience and time. However, it seems there is a reason to hope that a new vaccine won’t stay a fantasy forever.
Vaccine Proves Effective in HIV Trials
A research group in China completed pre-clinical HIV trials for a vaccine meant to prevent infection that women get from men. Not only did the vaccine prove effective, it performed better than expected. In an effort to confirm these findings, a group in the U.S. repeated the HIV trials, and added some rigorous testing. The results were the same, much to the delight of the scientists.
The vaccine in question was designed to protect women from seminal being transmitted to mucous membranes. In the studies, vaginal tissues were exposed to high viral loads – up to 70,000 times more than what is found in human semen. The vaccine was successful in warding off infection. Repeat exposure was tested as well. These also were fought off with the help of the vaccine. When they increased the viral amounts to 100,000 times the normal range, the immune system was overloaded and succumbed to the viral infection.
Experts are looking into how that might affect the vaccine — and ways to make it more potent. Another positive point that pleased the researchers was that certain environmental factors were inherently different between the two studies, yet the results yielded the same outcomes. The group is confident that with this confirming study, clinical HIV trials can proceed with little worry.
When and if that does happen, it could open doors for further vaccine testing and marketing. One other goal that has been in line with producing vaccines is designing them to be ingested instead of injected. The aim is to reach people in developing countries where resources may be limited.
Antibodies Produced by TLM B Cells Can’t Fight HIV Effectively
Finding a cure for HIV has led researchers from the National Institute of Health (NIH) to closely examine some of the unique circumstances associated with the condition. In recent tests, detailed information about TLM B cells and the formation of antibodies has come to light. The results show why many who are infected but receive no treatment for HIV, produce ineffective antibodies against the virus. Here is what they discovered.
What the Study Revealed About Antibodies in TLM B Cells
When a person is infected with HIV, and it goes untreated, the number of certain immune cells increases. The resting memory B cell is what typically resides in those with no infection. Once HIV has taken hold, this type of B cell declines in number, and the tissue-like memory B cell increases. What do these B cells do? How does this shift affect the fight against the HIV infection?
When a virus or another intruder infects the body, the TLM B cells will respond by dividing. These divisions produce antibodies specifically designed to attack the invader. The antibodies go through mutations along the way in an effort to become more effective. What researchers found, however, was that with HIV, the TLM B cells divided more than the resting memory cells. However, despite this, the antibodies that they produced did not mutate as much. Without the mutations, the virus proves no match for the antibodies. The resting memory B cells created efficient antibodies – just not enough to combat the infection.
Why This Study Is Important
This information is helping researchers understand why those with HIV seem unable to produce effective antibodies against the virus. Insight into this matter will aid the scientific community in coming up with new strategies to combat HIV and its spread. This discrepancy in the type of B cells a person has in his or her blood is just one of many important factors in the spread of HIV within a person’s body.