Posts tagged HIV therapy

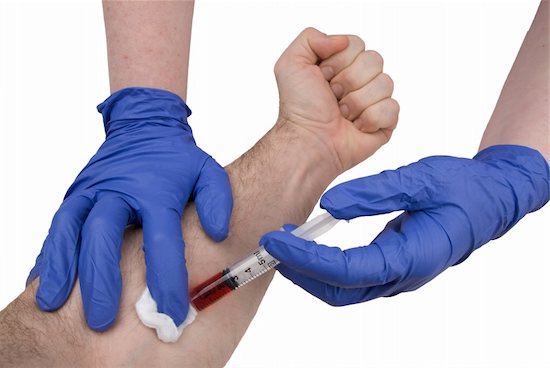
Nanotechnology May Improve HIV Medicines
Scientists and researchers focus on the improvement of HIV medicines in order to one day find a cure for the virus. Another reason the medical society puts so much effort into better medicine is to improve the lives of patients. In a new trial, the University of Liverpool has found success in using nanomedicine to potentially reduce the dosage of HIV treatment.
Using Nanotechnology for HIV Medicines
Nanotechnology is the process of making things on a smaller scale. That requires the manipulation of matter on the atomic, molecular, and supramolecular level. In nanomedicine, this means smaller, less expensive pills that work more effectively. This technology can change the way that future medicine is made.
The University of Liverpool’s Success
Both doctors and patients alike are hopeful for nanomedicine’s success. The University of Liverpool led a trial to prove the benefits of this type of medicine, with the intent to promote its usage within the scientific community.
The results from their trial showed that nanomedicine is far more effective. The body is able to absorb more of the drug. This means that patients can receive the same quality treatment and reduce the number of dosages they take. In fact, they found that patients could take potentially take half of the dosage and fight off the disease.
Today’s HIV therapies require daily doses just to keep up with the virus. This medicine can save HIV-positive individuals a significant amount of money on treatment. In certain countries where HIV is prevalent, this could mean better access to treatment by making the drugs more affordable.
Nanomedicine may also prevent non-adherence to therapy, which happens often when patients undergo the strain of taking medications daily. If the success of this trial can influence future HIV medicine, then this might prove great news for patients fighting against the virus. Hopefully, more research can lead to the technology’s implementation.
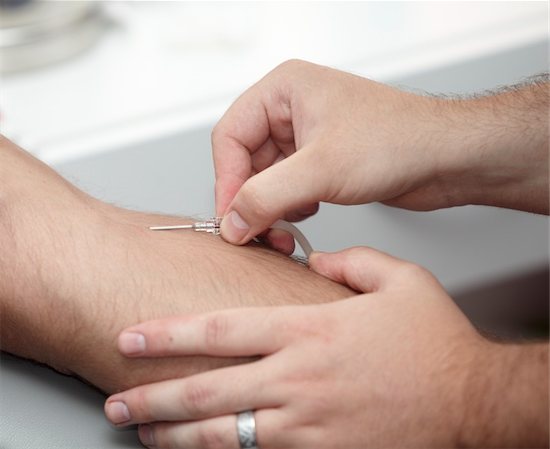
Beware of Dangerous ‘Shock and Kill’ Treatment for HIV
Finding effective treatment for HIV is a long-standing battle. Scientists are fighting against the disease every day. The search for answers may lead to drastic measures. However, at what point do the risk outweigh the cure? That’s the question posed by researchers at the Johns Hopkins University of Medicine when it comes to the ‘shock and kill’ treatment.
What is the ‘Shock and Kill’ Treatment for HIV?
The shock-and-kill treatment reveals HIV hidden within the cells. This is the problem that many scientists run into – HIV hides. When it is dormant, the virus does not trigger the immune system to fight back. It’s also the reason that antiretroviral therapies are only capable of keeping the disease at bay.
The proposed shock-and-kill treatment essentially wakes HIV from its dormant state to make it vulnerable to the immune system and antiretroviral drugs. However, testing this method has led scientists to believe the supposed ‘cure’ could have disastrous results.
The treatment was tested on the simian immunodeficiency virus (SIV), a disease that is found in primates and is very much similar to HIV. One of the test subjects displayed encephalitis symptoms and brain inflammation. The symptoms only worsened and the primate had to be put down humanely.
This treatment spells trouble if the disease is hiding within the brain. Activation in this area only makes a patient’s condition worse, especially when scientists do not know where the disease is hiding to begin with. Researchers advise caution.
“The potential for the brain to harbor significant HIV reservoirs that could pose a danger if activated hasn’t received much attention in the HIV eradication field,” says Janice Clements, Ph.D., professor of molecular and comparative pathobiology at the Johns Hopkins University School of Medicine. “Our study sounds a major cautionary note about the potential for unintended consequences of the shock-and-kill treatment strategy.”
Better Model Used to Further Development of HIV Vaccine
One of the best ways to stop the spread of disease is through vaccines. This long-used defense has halted numerous and dangerous infections over the years. It is no wonder then that scientists are urgently searching for ways to develop an HIV vaccine. A number of factors present obstacles that have, so far, stood in the way of progress.
3 Struggles in the Search for a HIV Vaccine
The menacing virus is an elusive microbe that evades detection both from the human immune system and most HIV vaccine models tested against it. What makes the virus so effective is the ability it has to mutate, which happen rapidly. Vaccines generally work by using non-infectious material and introducing it into the body where the immune system can identify and then attack it. The quickly changing virus means that a lesser amount of the virus is actually found and eliminated.
Another factor that gets in the way is the design of the HIV itself. The virus is packed into a type of envelope, which is coated with sugars that come from the host. Because this is on the outside of the microbe, it makes it difficult for the immune cells to identify it as an intruder.
A third issue in the mix is the lack of a living model that researchers can use to test potential HIV vaccines. This last obstacle has limited progress the most. Recent developments may finally change that.
A team of researchers has found that a certain species of primates has an immune system that closely resembles that of the human immune system. In order to be able to use this to their advantage, a virus that resembled HIV but that could infect the animal, had to be developed. The researchers, with some trial and error, were able to accomplish this. The result is a virus that infects and creates AIDS-like symptoms in the host animal. With a better model to test vaccines and monitor the viral envelope, they are hopeful to speed up HIV vaccine research and development.
New Study Clarifies the Link Between HIV and Tuberculosis
The link between HIV infection and the progression of other conditions is still a bit of a mystery. This is certainly the case when it comes to the body’s inability to keep in check the bacteria that causes tuberculosis, while in the presence of HIV. However, new insight into how the connection between the two conditions work, and how the immune system comes into play, has recently been published. This information could lead to further understanding of how to best treat the two conditions and support important immune system functions.
A large percentage of the population has the bacterium that develops into tuberculosis in their system. The immune system is generally quite adept at keeping the pathogen under control. For those who have this bacterium and are also infected with HIV, the tendency is to eventually develop tuberculosis as the HIV progresses. It was generally assumed that a weakened immune system, brought about by HIV infection, was the reason behind tuberculosis development in infected patients. This is not necessarily the case.
How HIV Progression Affects Tuberculosis in the Body
The published information painstakingly compared what was happening during each stage of HIV infection—with the effect on the immune system. What researchers found was that in the early stages of HIV infection, a function of the immune system diminishes. That component, called IL-10, is used to reduce inflammation. As HIV progresses, interferon response is noted. This is an antiviral immune response, but it dampens defense against tuberculosis.
The imbalance of immune support when the two infections are both present seems to be what accounts for the progression into tuberculosis. It should also be noted that other dangerous conditions can present suddenly in such an environment. Regulating the imbalance is what researchers are hoping to achieve as they continue to examine their findings. If successful, they will be able to modify the responses of the immune system to effectively combat both pathogens. This is important research as it relates to helping HIV-positive individuals to deal with secondary diseases as HIV progresses.
HIV Therapies According to Gender
The approach to treating HIV is similar for all—male and female, young and old. Adjustments can be made according to certain factors. A particular dosage may work for one, but may not be optimal for another. One recently published study shows why this can happen, and how medical professionals can increase the effectiveness of HIV therapies for their patients.
HIV Therapies and Gender
Preventing infection is an important part of curbing the spread of HIV. The drug used to prevent viral transfer is called Truvada. Until recently, it had been noted that the drug was most effective in men. Researchers found that it seemed less effective in women. Further investigation revealed that differences in tissues contributed to how well Truvada worked at preventing infection.
HIV needs access to genetic material in order to infect its host. The more DNA that is present, the stronger the viral hold. For women, vaginal and cervical tissues have more DNA present than in other types of tissue. Rectal tissue is also in this category. This requires considerable more medication to curtail HIV activity.
Armed with this knowledge, scientists mathematically calculated specific drugs-to-DNA ratios. Using this formula, and testing the outcomes, has proven successful. When increased doses were given to women, the rate of HIV infections decreased and more closely matched the male outcomes based on doses previously tried.
What does this mean for HIV therapies now? In short, women do best when taking Truvada every day. This contrasts considerably to the couple times a week generally prescribed. For the male population, the current dosage works well. Due to the anatomical differences, women require more of the medication. When taken daily, the rate of infection effectively decreases for this group. Of course, no one should change his or her therapy before consulting a healthcare provider.
So far, Truvada is the only FDA-approved pharmaceutical used to prevent the spread of HIV infections. Now with more information on how best to harness its potential, the medical world is in a good position to help keep others from contracting and spreading the virus.