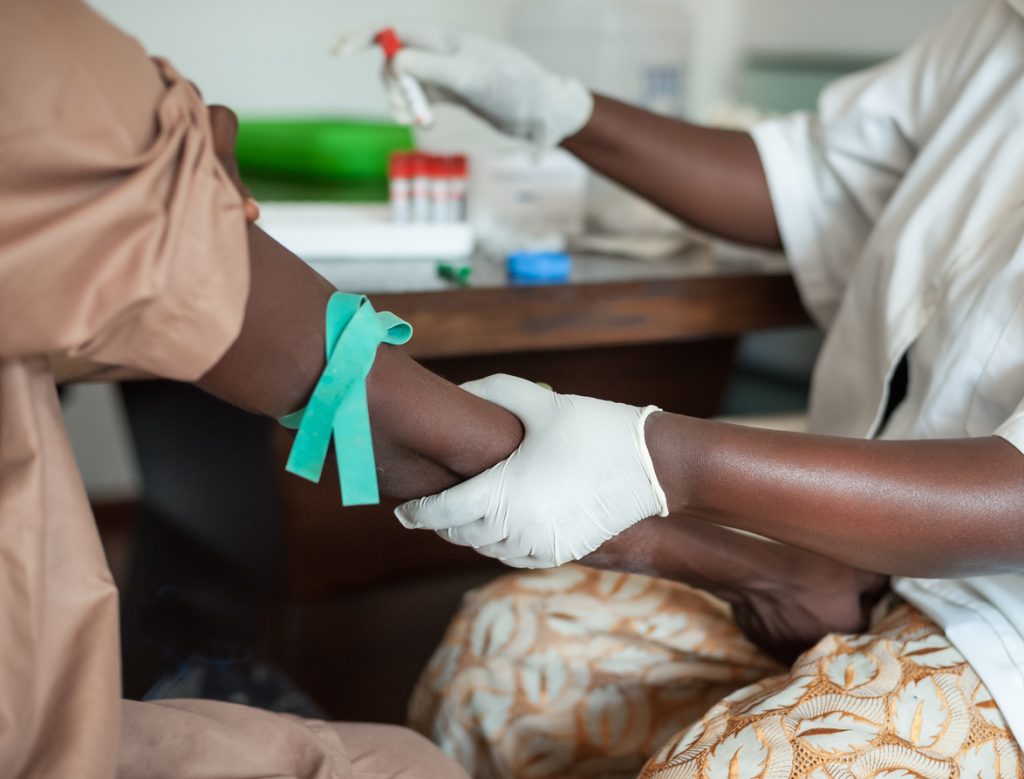
Posts tagged controlling HIV
The State of HIV Care in Europe
There were more than 2 million new infections in Europe and Central Asia, where they need better HIV care.
More than 35 million people are living with HIV/AIDS worldwide. This disease is an epidemic that affects other countries differently. For example, the prevalence of HIV in the Eastern and Southern Africa is high. These regions make up almost 50 percent of the total number of people living with HIV in the world. Access to HIV care in these parts of the world are scarce, leaving their population without much protection and an increasing number of new infections.
Other countries like Europe and Central Asia have seen a recent a drastic increase of new infections. Within the past couple of years, these regions saw a 57 percent increase in annual new HIV infections. Overall, there are 1.5 million people who live with HIV in Europe and Central Asia. To curb this rise, the European Centre for Disease Prevention and Control (ECDC) evaluated their method for combating HIV.
The Continuum of HIV Care
The ECDC developed a framework called the continuum of HIV care, which monitors the success of their HIV response. This framework involves looking at data from over 48 countries across Europe and Central Asia. The ECDC’s most recent report, the ECDC Dublin Declaration, looks at four aspects of HIV prevention, which it categorizes into stages:
- S1 – The estimated number of all people who live with HIV (PLHIV).
- S2 – The number of all PLHIV who have a diagnosis.
- S3 – The number on PLHIV who have a diagnosis and who are on ART.
- S4 – The number of PLHIV on ART who show signs of viral suppression.
The ECDC’s Findings
The ECDC saw an increase in the number of countries reporting data on all four stages of the continuum, from 40 percent to 66 percent. As more countries participate in the continuum, the ECDC can develop a better analysis of the state of HIV. Here’s the breakdown of their findings:
- 37 countries from Europe and Central Asia reported data for both Stage 1 and Stage 2.
- An estimated 1,199,000 people live with HIV, and 75 percent of those individuals have received a diagnosis.
- 1 in 4 people with a diagnosis is not receiving treatment for the disease.
- 31 countries from Europe and Central Asia reported data for both Stage 3 and Stage 4.
- 599,500 people with a diagnosis are using antiretroviral drugs, and only 88 percent show signs of viral suppression.
What the ECDC Learned
Efforts to monitor and predict the spread of HIV is only as great as the number of countries participating. As a result, the ECDC has trouble estimating the number of people living with HIV (Stage 1) and those who are virally suppressed (Stage 4). The organization hopes to support countries in using their modeling tool to develop better estimates of who has HIV and how many people show signs of viral suppression.
With more data, the ECDC can identify which countries need help fighting the infection, as well as improve testing, treatment, and HIV care. Hopefully, efforts by organizations like the ECDC and UNAIDS will be able to slow down and reverse the spread of HIV.
The Connection Between HIV and Osteoporosis
HIV is a crippling disease that slowly but surely tries to break down your body’s defenses. The virus compromises your immune system and your ability to fight off infections, leaving you vulnerable to the diseases of the world. One such condition includes osteoporosis.
Osteoporosis is a condition that affects both men and women over the age of 50. More than 4 percent of men and 16 percent of women over the age of 50 live with this disease in their femur neck or lumbar spine. To make matter worse, those with HIV are more likely to develop osteoporosis and scientist are unsure why.
How Osteoporosis Affects the Body
The bones are the structure and frame of our body, allowing us the ability to move. Strong and healthy bones are needed to keep the body upright, moving, and working properly. When osteoporosis strikes, the bones in our body begin to hollow out. This loss of bone density and mass causes bones to become weaker, leaving them susceptible to breakage.
Severe cases are known cause damage when a person sneezes or receives a minor bump. The longer a person has osteoporosis, the more likely they are to experience hip fractures, a collapsed vertebra, severe back pain, a loss of height, and spinal deformities.
How Are the Two Diseases Connected?
Over 54 million Americans live osteoporosis, while 1.2 million have HIV. Many studies show that the two disease are somehow connected. The loss of bone density occurs faster in those with HIV. What scientists don’t know is the exact cause. However, that hasn’t stopped them from trying to figure out why patients with HIV develop osteoporosis. The most common theories are the following:
- HIV medications.
- Long-term use of other medications like blood thinners, an antiseizure medicine, and corticosteroids.
- Old age.
- HIV infection.
What Symptoms Should You Look For?
Unfortunately, it can be hard to determine if you have osteoporosis unless you have broken a bone. This symptom the first sign of the disease. The U.S. Department of Health and Human Services (HHS) recommends bone density test for women over the age of 65, as they are the most at risk for the disease.
If you are HIV positive and over the age of 50, you should get tested as well. It’s important to look out for strain in your bones and joints, as well of any abnormal pain in those areas caused by a sudden bump or fall.
Preventing Osteoporosis
If you are HIV positive but do not have osteoporosis, there are measures that you can take to prevent the disease. A healthy diet will replenish the nutrients you need to maintain healthy bones. Be sure to eat plenty of foods with calcium and vitamin D. A healthy lifestyle will also slow the rate of bone loss. Exercise often and cut out bad habits like smoking and drinking alcohol. The most important thing that you can do is see your doctor or HIV specialist. An expert can guide you and the risk and steps to dealing with HIV and disease like osteoporosis.
Eliminating HIV in Sub-Saharan Africa Proves Difficult
We’ve discussed HIV’s impact on the sub-Saharan region of Africa before. Over the years, the disease has infected more than 25 million people, with the number of new infections rising every year. One the biggest obstacles the area faces is a lack of access to condoms. This contraceptive is rarely used among men and women in these countries. Eliminating HIV is no easy task, especially in a region where the prevalence of HIV is 1.5 times higher than Europe and the United States. The UN’s latest efforts to reduce the spread of the disease seems likely to fail.
Eliminating HIV in This Region Isn’t Easy
Organizations like the World Health Organization (WHO) and UNAIDS have found success in reducing the number of HIV patients in the United States and other similar countries. However, those countries are resource-rich areas, where they have the means and money to educate and distribute HIV protection. Both organizations have tried to implement similar efforts in the sub-Saharan region.
WHO and UNAIDS sought to use treatment as a prevention method. The plan would treat HIV-positive individuals and reduce their ability to infect others. They hoped to diagnose and treat 90 percent of the people within the next three years.
Why Researchers Cast Doubt
Unfortunately, a study by UCLA researchers cast doubt on this plan, seeing it as unfeasible. The researchers used statistical mapping to find people infected with HIV in Lesotho. At least 1 in 4 people have HIV in this South African country. Similar to other South African countries, most people have gone without a diagnosis, nor are they receiving treatment. The scientists discovered that the plan couldn’t address the fact that HIV-positive individuals are widely dispersed within the country. Also, very little of the population lives in urban areas, making it hard to find these people.
“Global health policies for HIV elimination need to be redesigned, and they need to consider settlement patterns and population density,” said Sally Blower, director of UCLA’s Center for Biomedical Modeling. “Our results show that the spatial demographics of populations in predominantly rural countries in sub-Saharan Africa will significantly hinder, and may even prevent, the elimination of HIV.”
“We estimate that almost every settlement in the country has at least one HIV-infected person, and this holds true for even the smallest and most remote settlement,” said Brian Coburn, the study’s other co-author, who was a postdoctoral fellow in Blower’s group. “We also found that approximately 70 percent of HIV-infected adults live in rural settlements.”
With those in need of treatment so widespread, it becomes harder and more expensive to help them. For every rural location, there is an average of two or fewer people per square kilometer who is HIV-positive. The problem is reaching them.
The Importance of Finding a Great Plan
The researchers at UCLA are using their technology to find alternate plans that address these issues. Blower states that in order “To develop effective strategies, we need to figure out — throughout entire countries — where HIV-infected individuals live and which communities are connected to each other.” Hopefully, whatever plan the governments of Africa chooses can curb the epidemic plaguing the continent and eventually help in eliminating HIV.

HIV Breakthrough Deciphers the Structure of the Virus
There is one question that has eluded scientists for so many years. How does HIV integrate into human host DNA and replicate in the body? More than a decade later, researchers have found the answer. An HIV breakthrough at the Salk Institute has deciphered the structure of HIV machinery.
Intasome: The Machinery Making Trouble
HIV intasome is a large molecular machine that adds viral DNA into the genomes of its host. This machinery is responsible for HIV’s elusive nature and its ability to hide within the body.
According to Dmitry Lyumkis, senior author, and fellow at the Salk Institute: “HIV is a clever virus and has learned to evade even some of the best drugs on the market. Understanding the mechanisms of viral escape and developing more broadly applicable drugs will be a major direction in the future.”
Scientists have come up with a way to combat intasome before by using a drug called integrase strand transfer inhibitors (INSTIs). It is approved to treat the virus in both the U.S. and Europe. However, the drugs and HIV machinery are a bit of a conundrum. Without being able to study intasome on the atomic level, the drug’s effects are not as powerful as it should be, leaving scientist stumped on how it should work.
How This HIV Breakthrough Was Made
New technology allows us to do better things. The same is true within the scientific community. The state-of-the-art imaging technique called the single-particle cryo-electron microscopy (cryo-EM) gave researchers the ability to image large, complex and dynamic molecules. Basically, they were able to see intasome structure clearly.
The molecular machine is composed of a four-part core but has many other complex parts to it. The researchers believe that this allows it to gain access to the cell’s nucleus through active transport instead of waiting for the cell to divide. Lyumkis calls for understanding each of these parts a bit more to combat the disease.

Heart Attack: HIV Patients at Nearly Double the Risk
Other than the brain, the heart is one of the most important organs in our body. It happens to also be a target for viruses like HIV. HIV positive individuals need to take caution and check on their heart regularly. A study shows that the risk for heart attack is much greater in those troubled by this disease.
Predicting Heart Attack Risk
The heart is vulnerable in America. At least, that is what the statistics say. Here are the facts that the CDC found:
- Every 43 seconds, someone in the United States has a heart attack.
- Every year, 735,000 Americans have a heart attack.
- Of those American, 525,00 are experiencing their first attack and 210,000 have experienced one before.
- One of 5 heart attacks is silent. This means that the patient is not aware it is happening but still suffers damage to the body.
These are truly awful facts. But what the scientists at the Northwestern University Feinberg School of Medicine have found may spell worse trouble for HIV patients. They are almost twice as likely to suffer from a heart attack, which more than what physicians have predicted for the general population.
Predicting the risk of heart attack is important. If a doctor discovers it early on, they can prescribe the right medicine to lower the risk. “If you have a higher risk for heart attack or stroke, your ability to benefit from one of these drugs is greater and justifies the possible side effects of a medication,” says Dr. Matthew Feinstein, cardiovascular disease fellow at Northwestern University.
Dr. Feinstein goes on to state that HIV increases heart risk by causing chronic inflammation, which can lead to plaque buildup in the body’s tissue. Eventually, this series of events in your body can lead to heart attack or stroke.
The current predictor tools for heart risk need to be adjusted. Heart medications are only given to those in serious need. If physicians cannot accurately tell if HIV patients need those medications, this will lead to dangerous consequences.